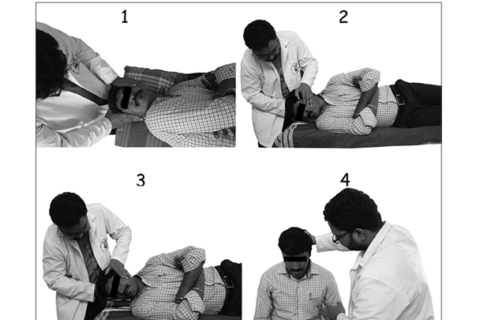
Outcome of Gans Repositioning Maneuver in Patients with Posterior Canal Benign Paroxysmal Positional Vertigo with Cervical Spondylosis
Published on: May 5, 2020
Indian Journal of Otology ¦ Volume 25 ¦ Issue 4 ¦ October-December 2019
H. Gayathri, Gurushekar Rose Preethi, Paul Mary P. Christina
Departments of ENT and Community Medicine, ACS Medical College and Hospital, Chennai, Tamil Nadu, India
Abstract
Background and Objectives: Cervical spondylosis and BPPV often co-exist in older population. As GRM doesn’t involve hyperextension of neck, which is better avoided among patients with cervical spine pathology, we decided to assess the outcome of GRM in patients with cervical spondylosis in terms of safety & efficacy. Methodology: Twenty patients with clinically proven posterior semicircular canal BPPV and radiologically evident cervical spondylosis without symptomatic spondylotic myelopathy or radiculopathy or severe restriction of neck or back movement were enrolled. GRM was done on the first day and repeated until resolution of nystagmus, for a maximum of four times. Lack of response to GRM even after fourth attempt was considered as failure. The manuever was repeated in the successful group on day two and after one week & these patients were followed up for one month. Results: Overall, 75% of the patients (50.9% to 91.3% – 95% C.I.) had a successful repositioning maneuver. Favourable parameters for better chances of cure were higher age (>55 years), male gender & higher grade of cervical spondylosis. 20% of patients had experienced temporary pain for few hours on the day of maneuver. None of the patients who had less than two attempts of GRM had post-procedure pain. Clinically, none of the patients had precipitation of cervical myelopathy or radiculopathy. Conclusion: GRM is a safe & effective particle repositioning maneuver for patients with posterior semicircular canal BPPV
with co-existent cervical spondylosis.